Answer: Disseminated strongyloidiasis
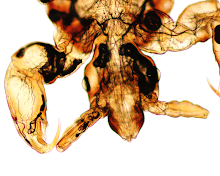
Shown is a very heavy infection of Strongyloides stercoralis, with numerous larvae seen in this sputum specimen. When we identify Strongyloides in my lab from any specimen outside of the GI tract, we consider it a critical result and report it to the physician immediately. Unfortunately, this case was fatal, despite prompt treatment.
As Lukus points out, "Disseminated strongyloidiasis, can occur in patients immunosuppressed by chemotherapy or AIDS; Ivermectin is treatment of choice."
Of note, a low level of autoinfection occurs naturally in immunocompetent hosts, during which filariform larvae enter the circulation and travel to the lungs. They then break out into the airways, migrate up the bronchi and trachea, and then are swallowed, to reach the small intestine where they mature into adults. This is how infection can persist for decades. Unfortunately, an immunocompromised state can accelerate this process, resulting in large numbers of larvae entering the circulating and traveling to the lung and elsewhere in the body. Death is often due to sepsis (due to bowel flora carried by the larvae into the blood and CSF) and respiratory failure.
Sunday, July 21, 2013
Subscribe to:
Post Comments (Atom)


2 comments:
Shouldn't the patient be screened for Strongyloïdes before treatment ?
I've seen a few cases before and they all ended up in death of the patient.
Hans Naus
Yes, it is generally considered best practice to screen patients coming from endemic areas or with a significant travel history, prior to starting any type of immunosuppressive therapy. However, sometimes the travel history is not obtained - especially when the travel was a long time ago, as was the case in this patient.
Post a Comment