A 90-year-old male from Missouri presented with a 3-day history of fever and dyspnea. His medical history included hypertension and splenectomy due to injury. He lived with his wife and reported no recent travel, pet or known tick exposure.
On admission, he was febrile (temperature 40˚C) and hypotensive (105/58). Laboratory values of note were elevated leukocytes (13,100 cells/mL; 58% neutrophils), decreased hemoglobin (9.5 g/dL), low platelet count (106,000 cells/mL), increase liver function tests (total bilirubin 3.2; alkaline phosphatase 45 units per liter; aspartate transaminase 1935 units per liter; alanine transaminase 872 units per liter). Chest radiographs on admission were clear, but repeat testing on the following day showed new right lung airspace opacities. Empiric antibiotics were begun with vancomycin and moxifloxacin, but he experienced increasing hypotension and dyspnea. Based on a suspicion for tickborne disease, an EDTA whole blood sample was submitted for microscopic examination and real-time PCR for Ehrlichia/Anaplasma and Babesia microti.
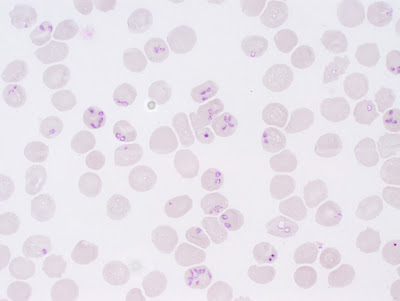
The Babesia microti PCR was negative, as well as a multiplex PCR for Ehrlichia ewingii, E. chaffeensis, and Anaplasma phagocytophilum, but the giemsa-stained, peripheral blood thin films showed the following (CLICK ON IMAGES TO ENLARGE):
Repeat Babesia microti PCR was still negative and malaria PCR (done for investigative purposes) was also negative.
What is your diagnosis? How would you further work up this case?







14 comments:
other Babesia species like B. divergens.
Agree with Babesia. Great shots of Maltese crosses!
The small rings, together with Maltese crosses, a history of splenectomy and negative testing for B. microtti, all points toward Babesia sp. most likely B. divergens.
I can't believe that there are two respondents before me, such dedicated scientists.
Florida fan
Babesia spp. Beautiful smears! I don't think any additional work-up is needed but if necessary I would look for a lab with a Babesia PCR that is genus specific only and sequence the product to confirm the species.
Agree, definitely Babesia sp. I wonder if serology (perhaps more broadly specific??) and an attempt to culture would be useful . . .
Babesia sp. not microti..probably MO1?
Lee
Babesia - maltese crosses give it away (are there some extracellular merozoites too?)
maybe do a B. divergens PCR, as although the patient reports no travel to Europe, and B. divergens cases in humans are rare, I read that the most severe infections, beyond that of flu like fever, are observed in asplenic patients...
Agree with babesia and also think that MO1 is a good consideration, especially since this patient is from Missouri!
Another really cool case and I vote worthy of #250. I will be curious as to the logic of picking this vs some totally grossly offensive worm etc.
I would have guessed babesia also so have nothing to offer diagnostically but am going to guess the rest of the history will be "and the patient died".
I'll be curious if this was missed on the orginal CBCs, why, and if any tip-offs to trap something like this if an automated diff etc.
I would say this is not Plasmodium, I am not expert in Babesia but would conioder this for my disgnosis.
Would Parasite Gal mention Babesia and PCR when the answer is Babesia? For special case #250? I know nothing about human pathology, but quite a bit about composing tests for students. I'll vote "not Babesia" based purely on the syntax of the blog entry.
--bks
Agree with Babesia sp. other than microti. Maltese crosses seen on smear. No further testing?
I vote Babesia as well. If this were a Plasmodium infection, you would see late stages on the smear (patient is splenectomized). Only rings and Maltese Crosses are present.
Viruse B or C infection.
Post a Comment